Managing unpleasant symptoms and changing your lifestyle drastically – living with a chronic illness is challenging. But it needn't break you down. James Frew explains how mindfulness and meditation has given him the resilience to thrive while living with a long-term condition...
All it took was a fall in the middle of a road to realize something was wrong.
It was July 2013 and I'd just returned from a month-long overseas business trip. I was tired, unable to think properly, and was regularly physically sick after eating. But it wasn't until that moment on the road outside the office that I became convinced this wasn't just a severe case of jet lag.
The following day, I visited the doctor and so started months of tests, false starts, and inconclusive assessments. It wasn't until January 2014 that I received an official diagnosis of Postural Orthostatic Tachycardia Syndrome (POTS). All the while, I'd been away from work, barely able to leave the house, with my symptoms worsening.
Although there was relief in the diagnosis – finally having a name for the ensemble of seemingly unrelated symptoms – it was much more the beginning than the end. Truthfully, it was the start of living with chronic illness and pain.
Learning to live with Dysautonomia
A lot of people would say that living with a chronic illness is quite an isolating experience. That's certainly how I felt, especially in the first few years of my condition. The symptoms of POTS, a form of dysautonomia or autonomic dysfunction, vary significantly between individuals and fluctuate on a daily and sometimes even hourly basis. For me, unpredictability was, and still is, one of the most demanding challenges to overcome.
When in the middle of an extreme flare-up of symptoms, it's difficult to communicate to others how you're feeling, particularly when suffering from the cloudiness of brain fog. For many years, I couldn't work because of the debilitating cognitive effect this had on me. Some people say it feels like having cotton wool in your brain; you're aware there's something there, but it's hard to find clarity in it.
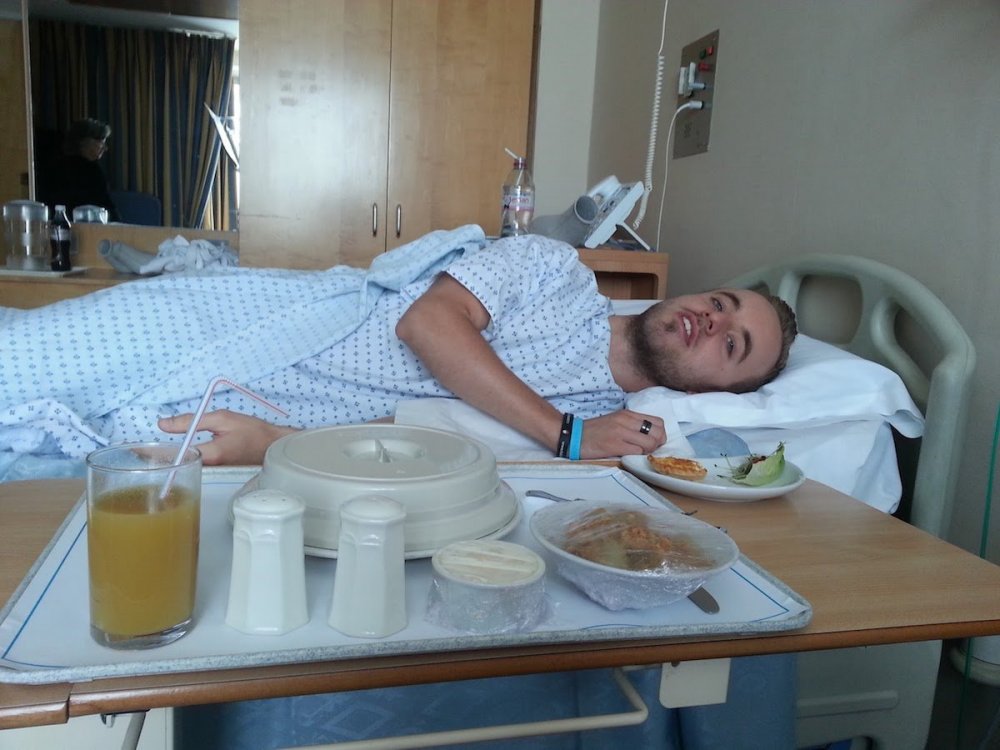 James lives with the chronic condition POTS
James lives with the chronic condition POTS
This isn't uncommon for POTS patients, either. According to Dr. Lesley Kavi, Visiting Professor at Birmingham City University and Trustee and Chair of the charity PoTS UK, the most debilitating symptom of POTS “varies very much from person to person depending on the set of symptoms they have. I read many comments that say the brain fog is the worst, but not everyone says this.”
This is typical when discussing chronic illnesses. Like the common cold, some illnesses are short-lived and unpleasant; chronic illnesses, though, don't have a known end-point. Although there's no way to say for sure, I'll probably experience POTS symptoms for the foreseeable future. While some people find their condition naturally resolves, Dr. Kavi notes that many, “especially those with inherited conditions that cause [POTS], can have symptoms long-term.”
Living with chronic illness
Chronic illnesses are generally defined as long-term conditions with no cure. However, there's no one accepted definition of a chronic illness, so its hard to get an accurate measure of how many people suffer with a long-term condition. The US Centers for Disease Control and Prevention (CDC) opts for the term chronic disease, and estimates that six in ten adults have a long-term condition which affects their daily lives.
Often, the symptoms are wide-ranging, diverse and unpredictable. As a result, living with chronic illness can sometimes feel like a continual trial. For every positive moment, there are a handful of upsetting, distressing, or frustrating ones. Following the onset of my illness, I found it particularly hard to come to terms with how different my life now was. Even simple things like going out of the house require effort and preparation.
“Often, the symptoms are wide-ranging, diverse and unpredictable. As a result, living with chronic illness can sometimes feel like a continual trial. For every positive moment, there are a handful of distressing or frustrating ones.”
It's not helped that I tend not to look any different outwardly. The effects of POTS are primarily internal, like a sudden increased heart rate, low blood pressure and digestive issues. This type of condition is usually referred to as an invisible illness, a common trait of many chronic illnesses. As a previously well man in his early 20s when POTS first took hold, most people couldn't see the suffering I was going through.
As a result, I was nervous about going out and anxious about how people may interact with me if I need to sit down on a busy bus or train or use an accessible toilet. Most days, I still feel this way. I know I tend to shy away from spontaneity, preferring low-key plans instead. But after so many years living with chronic illness, I've become used to accepting my difference.
Meditation to calm anxious thoughts
There wasn't an overnight transformation; I didn't wake up one morning comfortable in my skin and ready to take on the world. It was a gradual process over many years, continually chipping away at the biases and thought patterns from before. But I didn't do it alone, either. After reading about a meditation app online, I ignored my misplaced skepticism about the practice and gave it a go.
RELATED: Do mindfulness apps work?
In the years since, I've spent at least ten minutes a day training my mind to be comfortable with feelings and learning that I am not my thoughts and I'm not defined by my condition. Where I used to spend long periods worrying about what people may think, I've come to accept that these are the musings of an anxious mind concerned about a future that may never happen. This regular practice has also helped me feel connected to others, even while physically alone.
Although you might never meet them in person, the internet offers a way to connect with other people living with chronic illness around the world. I've spent many hours in the /r/POTS subreddit chatting, learning, and supporting the newly-diagnosed.
In fact, the benefits of this type of interaction were confirmed by a 2016 study published in Qualitative Health Research, which found that online communities strengthened relationships, exchanged knowledge, and raised awareness about specific illnesses.
Finding ways to manage chronic pain
My meditation practice meant that I could focus on the present moment, rather than the future or the past. But is also helped manage the chronic pain caused by POTS in combination with Ehlers Danlos Syndrome (EDS), a connective tissue disorder. The pain still exists, of course, but it is my reaction to it that has changed. Chronic pain is a highly challenging condition to live with. My personal experience hasn't been overwhelming, but an underlying current of long-term pain.
RELATED: 9 science-backed benefits of meditation
However, it can be extremely debilitating for many people suffering from it. As the mechanisms behind this agony aren't yet understood, treatments are variable, and some find them ineffective. Still, there's growing evidence, like the meta-study published in the Annals of Behavioral Medicine in 2016, that a regular meditation practice can help make living with chronic illness and long-term pain more manageable.
Coping with mental health and chronic illness
Meditation is just one technique I've come across to ease the difficulty of living with chronic illness. As Dr. Kavi points out, "it can be a challenge to cope with the fluctuations; some people don't need help with [their] mental health, some gain benefit from psychological therapies including CBT [or] mindfulness, and some have medication."
Although mindfulness has been the most successful for me, it didn't happen in isolation. Not long after my diagnosis, I was prescribed SSRI-based anti-depressants to help manage my mental health. Alongside this, I took a Cognitive Behavioral Therapy (CBT) course and followed that up with counseling.
“There's growing evidence that a regular meditation practice can help make living with chronic illness and long-term pain more manageable.”
Everyone's experience is different, but the key to living with chronic illness is to do what's right for you. These therapies and techniques were effective for me, but they might not be for everyone. You may find it's worth exploring your options with a healthcare professional.
Working around your condition
In an alternative world, we might be able to spend our days living with chronic illness, managing experiences at our own pace. But in many cases, there's still a financial imperative to work. Alongside this, after a few years of relative monotony, I wanted to have something practical to achieve.
But, given the unpredictable, long-term nature of chronic illness, most don't feel able to return to full-time employment in an office or workplace away from home. There are alternatives to explore, though, even if they are less conventional.

James is proof you can thrive with a chronic illness
Some people turn their hobbies into a part-time business, allowing them to bolster their finances without the pressure of working all the time. This was the approach that led to my return to work. Writing started as a hobby before becoming part-time job, and then, years later, a career.
But that's far from the only way to earn while living with chronic illness. If you do feel comfortable returning to an office, it's worth finding an understanding employer to accommodate the adjustments you need. The important thing is to do what you feel comfortable with, and at your own pace.
Over the years, my illness has given me a chance to connect with my body in a way I'd never imagined. While the struggle is real, I've come to accept that this is who I am now, and in many ways, I'm better for it.
After almost a decade, living with chronic illness is still a work in progress. My experience evolves each day, but so do I. For every setback, I have an opportunity to learn from it. For each day spent recovering from the onset of symptoms, I find comfort knowing that tomorrow may be different.
happiness.com | The fine art of being: learn, practise, share
Are you a happiness.com member yet? Sign up for free now to enjoy:
■ our happiness magazine with practical life tips
■ share and support others in our happiness forum
■ develop with free online classes in our happiness Academy
Written by James Frew
 James is a freelance writer based in the UK with a focus on consumer technology, mental health, well-being, and sustainability. When not writing, he's usually listening to podcasts, enjoying music, or going for a walk. You can find all his work on Campsite.bio and follow him on Twitter.
James is a freelance writer based in the UK with a focus on consumer technology, mental health, well-being, and sustainability. When not writing, he's usually listening to podcasts, enjoying music, or going for a walk. You can find all his work on Campsite.bio and follow him on Twitter.

Join the conversation
You are posting as a guest. If you have an account, sign in now to post with your account.
There are no comments to display.